[0013]To improve the safety of
hospitalized patients, particularly those in lower-acuity areas, it is desirable to have a body-worn monitor that continuously measures all vital signs from a patient, provides tools for effectively monitoring the patient, and wirelessly communicates with a hospital's
information technology (IT) network. Preferably the monitor operates algorithms featuring: 1) a low percentage of false positive alarms / alerts; and 2) a high percentage of true positive alarms / alerts. The term ‘alarm / alert’, as used herein, refers to an audio and / or visual alarm generated directly by a monitor worn on the patient's body, or alternatively a remote monitor (e.g., a central
nursing station). To accomplish this, the invention provides a body-worn monitor that measures a patient's vital signs (e.g. cNIBP, SpO2, HR, RR, and TEMP) while simultaneously characterizing their activity state (e.g. resting, walking, convulsing, falling) and posture (upright, supine). The body-worn monitor processes this information to minimize corruption of the vital signs and associated alarms / alerts by motion-related artifacts.
[0014]The body-worn monitor features a
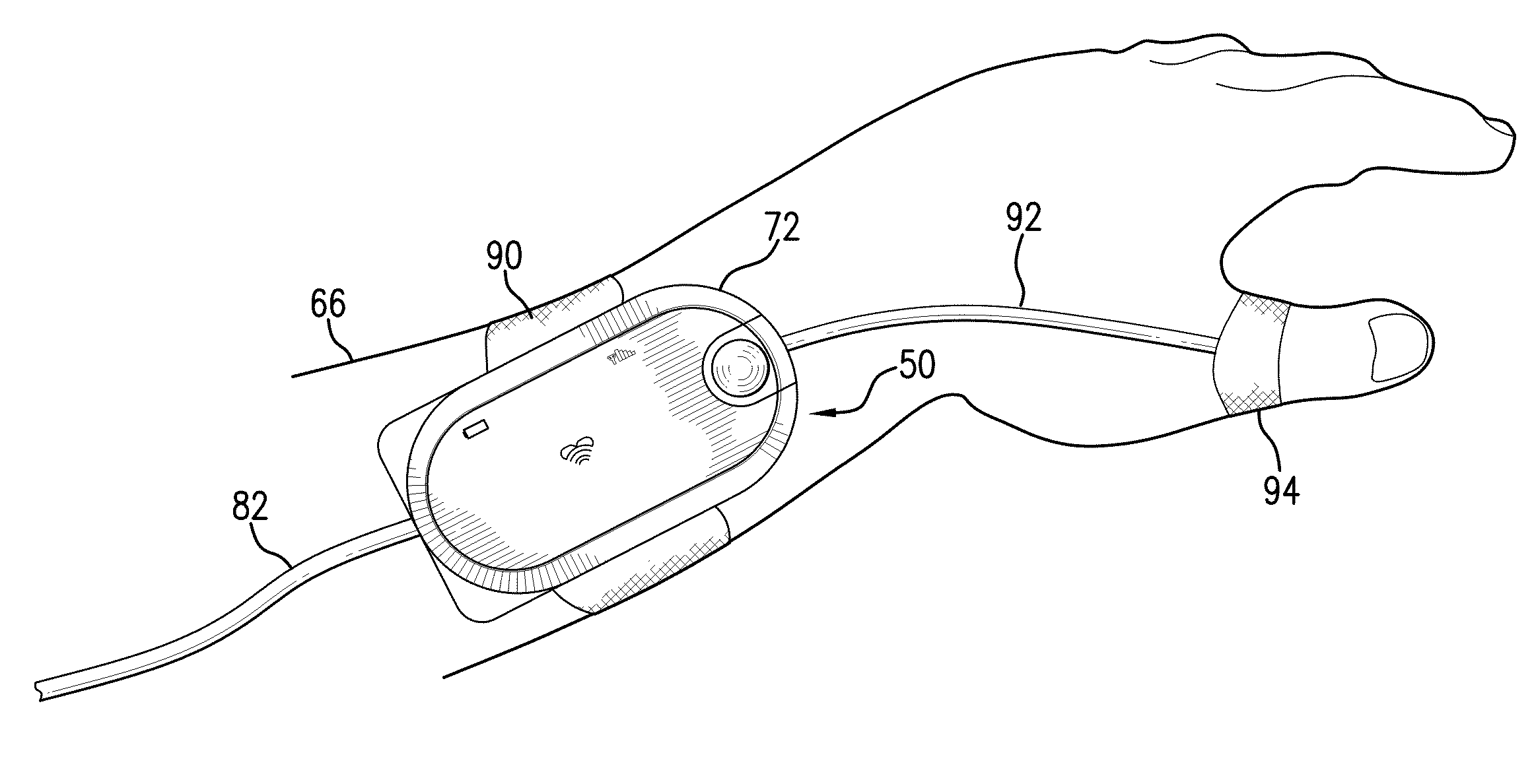
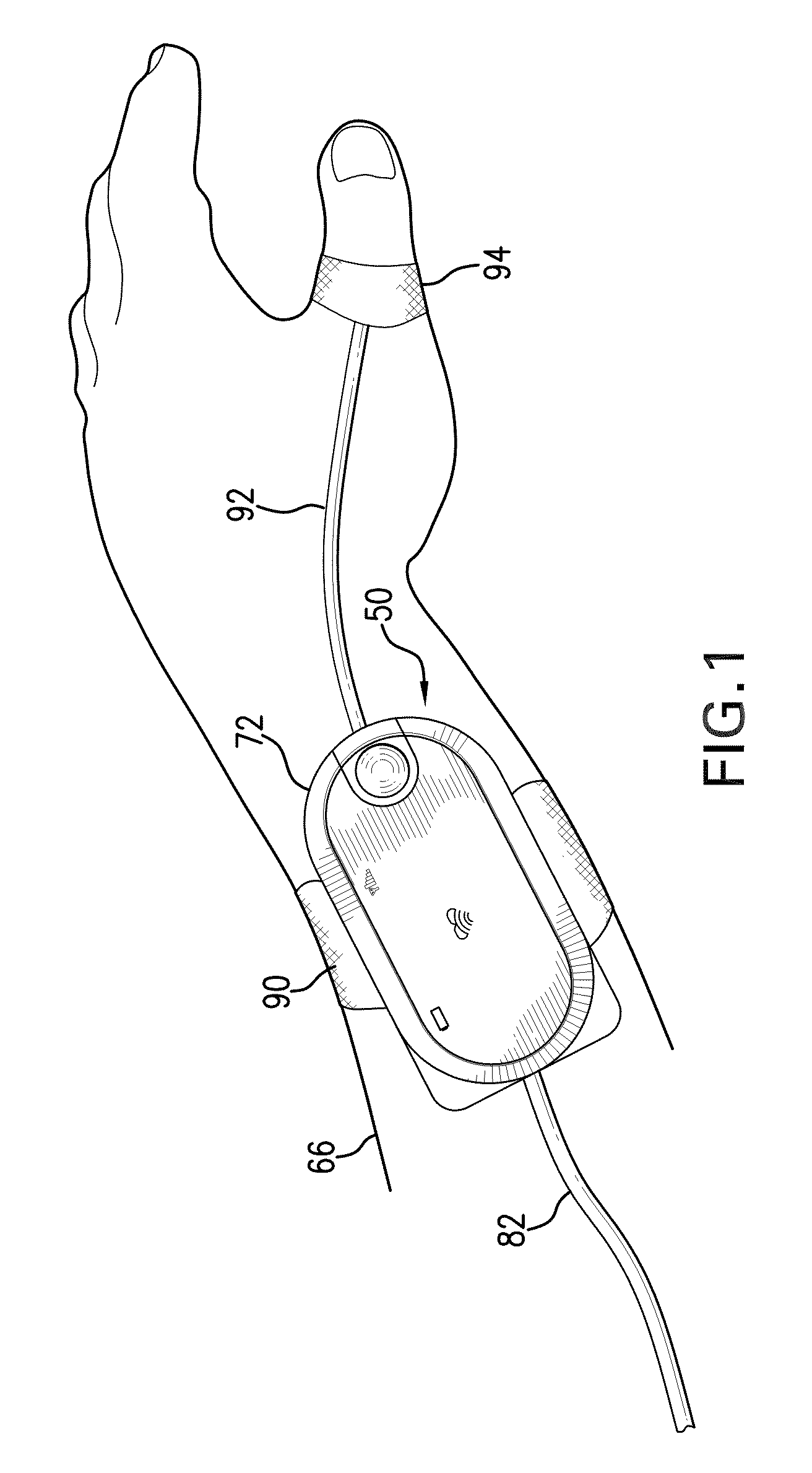
graphical user interface (GUI) rendered on a touchpanel display that facilitates a number of features to simplify and improve patient monitoring and safety in both the hospital and home. For example, the monitor features a battery-powered,
wrist-worn
transceiver that processes motion-related signals generated with an internal motion sensor (e.g. an
accelerometer). When the
transceiver's battery runs low, the entire unit can be swapped out by simply ‘bumping’ the original
transceiver with a new one having a fully charged battery. Accelerometers within the transceivers detect the ‘bump’, digitize the corresponding signals, and wirelessly transmit them to a
patient data server (PDS) within the hospital's network. There, the signals are analyzed and
patient information (e.g. demographic and vital sign data) formerly associated with the original transceiver is re-associated with the new transceiver. A clinician can view the data using a computer functioning as a remote viewing device (RVD), such as a conventional computer on wheels (COW).
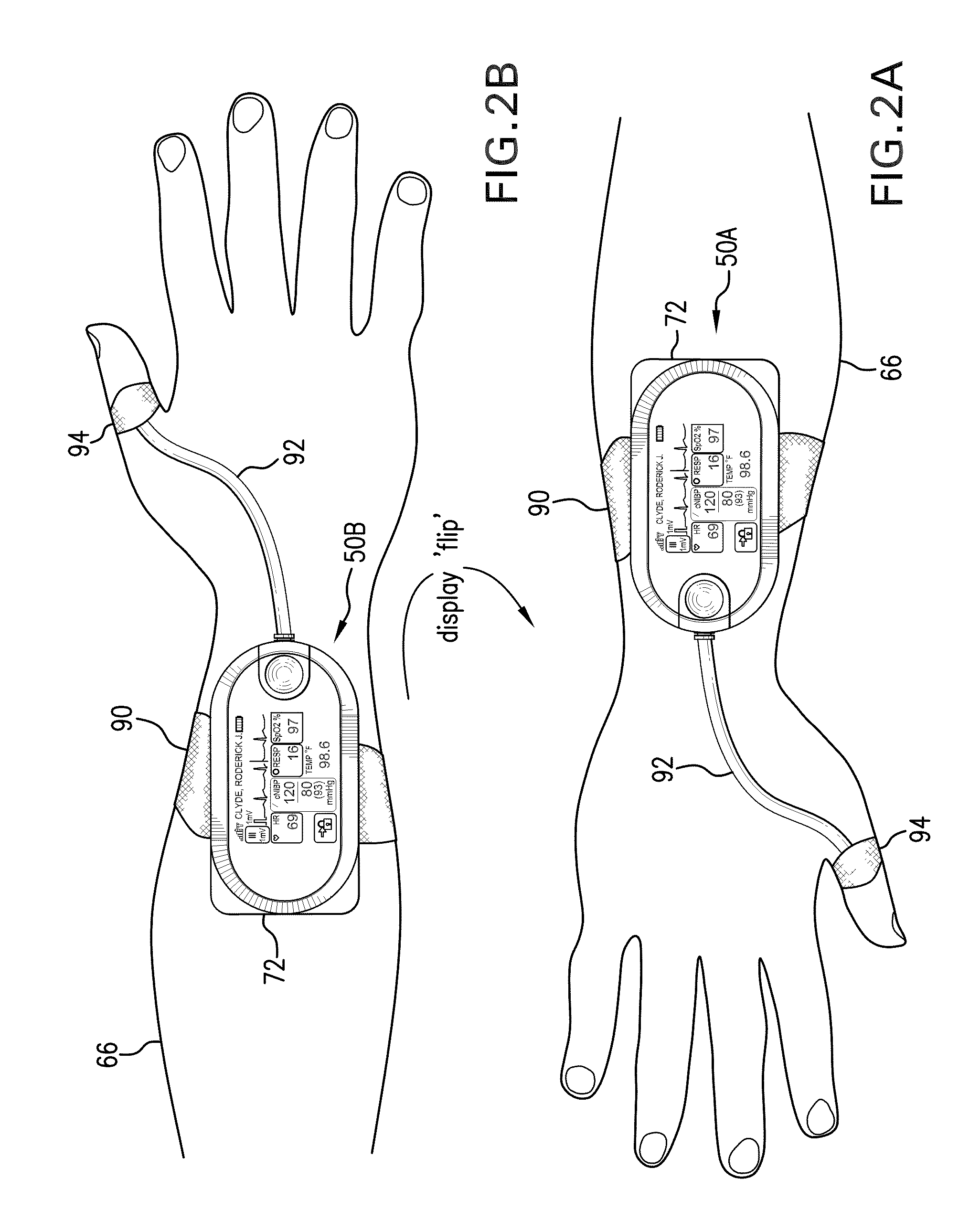
[0018]The
wrist-worn transceiver's touchpanel display can render a variety of different GUIs that query the patient for their
pain level, test their degree of ‘mentation’, i.e.
mental activity, and perform other functions to assist and improve diagnosis. Additionally, the transceiver supports other GUIs that allow the patient to order food within the hospital, change the channel on their television, select entertainment content, play games, etc. To help promote safety in the hospital, the GUI can also render a photograph or video of the patient or, in the case of neo-natal patients, their family members.
[0020]The body-worn monitor features a series of sensors that attach to the patient to measure time-dependent PPG, ECG, ACC, oscillometric (OSC), and impedance pneumography (IP) waveforms. A
microprocessor (CPU) within the monitor continuously processes these waveforms to determine the patient's vital signs, degree of motion, posture and
activity level. Sensors that measure these signals typically send digitized information to the
wrist-worn transceiver through a serial interface, or
bus, operating on a controlled
area network (CAN) protocol. The
CAN bus is typically used in the
automotive industry, and allows different
electronic systems to effectively and robustly communicate with each other with a small number of dropped packets, even in the presence of electrically noisy environments. This is particularly advantageous for ambulatory patients that may generate signals with large amounts of motion- induced
noise.
 Login to View More
Login to View More  Login to View More
Login to View More