Medical Devices, Drug Coatings and Methods for Maintaining the Drug Coatings Thereon
- Summary
- Abstract
- Description
- Claims
- Application Information
AI Technical Summary
Benefits of technology
Problems solved by technology
Method used
Image
Examples
example 1
[0111] A PVDF homopolymer (Solef® 1008 from Solvay Advanced Polymers, Houston, Tex., Tm about 175° C.) and polyfluoro copolymers of poly(vinylidenefluoride / HFP), 92 / 8 and 91 / 9 weight percent vinylidenefluoride / HFP as determined by F19 NMR, respectively (eg: Solef® 11010 and 11008, Solvay Advanced Polymers, Houston, Tex., Tm about 159 degrees C. and 160 degrees C., respectively) were examined as potential coatings for stents. These polymers are soluble in solvents such as, but not limited to, DMAc, N,N-dimethylformamide (DMF), dimethyl sulfoxide (DMSO), N-methylpyrrolidone (NMP), tetrahydrofuran (THF) and acetone. Polymer coatings were prepared by dissolving the polymers in acetone, at five weight percent as a primer, or by dissolving the polymer in 50 / 50 DMAc / acetone, at thirty weight percent as a topcoat. Coatings that were applied to the stents by dipping and dried at 60 degrees C. in air for several hours, followed by 60 degrees C. for three hours in a <100 mm Hg vacuum, resulted...
example 2
[0112] A polyfluoro copolymer (Solef® 21508) comprising 85.5 weight percent vinylidenefluoride copolymerized with 14.5 weight percent HFP, as determined by F19 NMR, was evaluated. This copolymer is less crystalline than the polyfluoro homopolymer and copolymers described in Example 1. It also has a lower melting point reported to be about 133 degrees C. Once again, a coating comprising about twenty weight percent of the polyfluoro copolymer was applied from a polymer solution in 50 / 50 DMAc / MEK. After drying (in air) at 60 degrees C. for several hours, followed by 60 degrees C. for three hours in a <100 mtorr Hg vacuum, clear adherent films were obtained. This eliminated the need for a high temperature heat treatment to achieve high quality films. Coatings were smoother and more adherent than those of Example 1. Some coated stents that underwent expansion show some degree of adhesion loss and “tenting” as the film pulls away from the metal. Where necessary, modification of coatings c...
example 3
[0114] Polyfluoro copolymers of still higher HFP content were then examined. This series of polymers were not semicrystalline, but rather are marketed as elastomers. One such copolymer is Fluorel™ FC2261Q (from Dyneon, a 3M-Hoechst Enterprise, Oakdale, Minn.), a 60.6 / 39.4 (wt / wt) copolymer of vinylidenefluoride / HFP. Although this copolymer has a Tg well below room temperature (Tg about minus twenty degrees C.) it is not tacky at room temperature or even at sixty degrees C. This polymer has no detectable crystallinity when measured by Differential Scanning Calorimetry (DSC) or by wide angle X-ray diffraction. Films formed on stents as described above were non-tacky, clear, and expanded without incident when the stents were expanded.
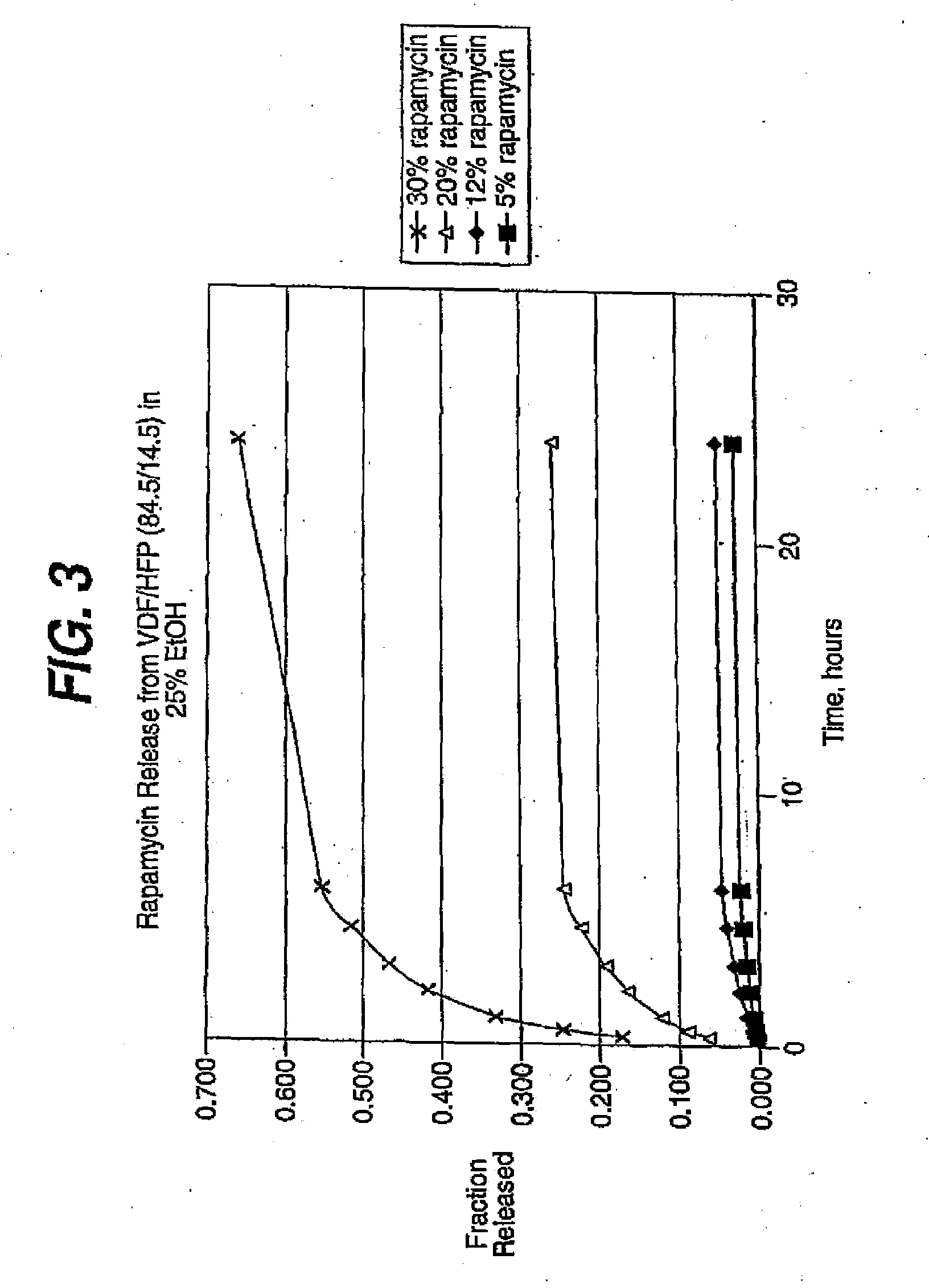
[0115] The coating process above was repeated, this time with coatings comprising the 60.6 / 39.4 (wt / wt) (vinylidenefluoride / HFP) and about nine, thirty and fifty weight percent of rapamycin (Wyeth-Ayerst Laboratories, Philadelphia, Pa.), based on total we...
PUM
| Property | Measurement | Unit |
|---|---|---|
| Temperature | aaaaa | aaaaa |
| Temperature | aaaaa | aaaaa |
| Fraction | aaaaa | aaaaa |
Abstract
Description
Claims
Application Information
 Login to View More
Login to View More - R&D Engineer
- R&D Manager
- IP Professional
- Industry Leading Data Capabilities
- Powerful AI technology
- Patent DNA Extraction
Browse by: Latest US Patents, China's latest patents, Technical Efficacy Thesaurus, Application Domain, Technology Topic, Popular Technical Reports.
© 2024 PatSnap. All rights reserved.Legal|Privacy policy|Modern Slavery Act Transparency Statement|Sitemap|About US| Contact US: help@patsnap.com